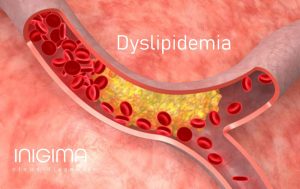
Dyslipidemia and CVD risk factors
When someone’s blood lipid levels are abnormal, they are said to have dyslipidemia.
Although there are several disorders that fall under this umbrella category, dyslipidemia most frequently involves:
- High levels of bad cholesterol, or low-density lipoproteins (LDL),
- Low levels of HDL (good cholesterol), or high-density lipoproteins
- High triglyceride levels
- High LDL and triglyceride levels, often known as high cholesterol
Lipids, often known as fats, are essential for life and give cells energy. Lipids consist of:
LDL cholesterol is viewed negatively because it can lead to blood vessel plaque formation.
Because it can assist in removing LDL from the circulation, HDL cholesterol is viewed as being of good quality.
Triglycerides are fatty acids that form when calories are not immediately consumed and are kept in fat cells.
Normal blood lipid levels differ from person to person inherently. However, those who have very low HDL levels or high levels of LDL and triglycerides are more likely to develop atherosclerosis.
Plaques, which are solid, fatty deposits that restrict blood flow, build up in blood vessels and cause atherosclerosis.
These plaques have the potential to accumulate over time and result in serious circulation issues like heart attacks and strokes.
Symptoms
Most people who have dyslipidemia are not aware of it unless it is severe. Typically, dyslipidemia is identified by a doctor during a normal blood test or a screening for another condition.
Peripheral artery disease (PAD) and coronary artery disease (CAD) are two more disorders that can develop from severe or untreated dyslipidemia (PAD).
Heart attacks and strokes are just two of the significant health issues that CAD and PAD can lead to. These conditions’ typical signs and symptoms include:
- Leg Pain, Especially When Walking Or Standing
- Chest Pain
- Tightness Or Pressure In The Chest And Shortness Of Breath
- Pain, Tightness, And Pressure In The Neck, Jaw, Shoulders, And Back
- Indigestion And Heartburn
- Sleep Problems And Daytime Exhaustion
- Dizziness
- Heart Palpitations
- Cold Sweats
- Vomiting And Nausea
- Swelling In The Legs, Ankles, Feet, Stomach, And Veins Of The Neck
- Fainting
“It’s strongly recommended by the Doctors to maintain the symptoms recorded in INIGIMA Cloud Diagnosis which helps to understand the patient trend and variation of health.”
Causes and types
According to the underlying cause, there are two forms of dyslipidemia:
First-stage Primary dyslipidemia
Primary dyslipidemia is caused by genetic causes and is inherited. The following are typical causes of primary dyslipidemia:
Familial mixed hyperlipidemia, which can cause excessive cholesterol and occurs in adolescents and young adults.
A mutation in a class of LDL lipoproteins known as apolipoproteins causes familial hyperapobetalipoproteinemia.
High triglyceride levels are caused by familial hypertriglyceridemia.
A mutation in the LDL receptors causes homozygous familial or polygenic hypercholesterolemia.
Secondary dyslipidemia
Lifestyle choices or medical circumstances that affect blood lipid levels over time might result in secondary dyslipidemia.
The following are typical causes of secondary dyslipidemia:
Diabetes, Particularly Extra Weight Around The Waist, And Obesity
Hypothyroidism
Alcoholism Is Another Name For Alcohol Use Disorder.
Ovarian Polycyst Syndrome
The Metabolic Syndrome
High Dietary Fat Consumption, Particularly Of Saturated And Trans Fats
Cushing’s Disease
IBS, Also Known As Inflammatory Bowel Disease, Serious Infections Like HIV, And Abdominal Aortic Aneurysm
Risky components
It is well-recognised that a number of variables raise the risk of dyslipidemia and associated disorders.
These risk elements consist of:
- Obesity
- A Sedentary Lifestyle
- A Lack Of Regular Physical Exercise
- Alcohol Use
- Tobacco Use
- Use Of Illegal Or Illicit Drugs
- STD Sexually Transmitted Infections
- Type 2 Diabetes
- Hypothyroidism
- Chronic Kidney Or Liver Conditions
- Digestive Conditions
- Older Age
- A Diet Rich In Saturated And Trans Fats
- A Parent Or Grandparent With Dyslipidemia
- Female Sex, As Women Tend To Experience Higher LDL Levels After Menopause
Treatment Guideline
A physician will often concentrate on reducing a patient’s triglyceride and LDL levels. The underlying cause of dyslipidemia and the severity of the condition will determine the best course of action.
For patients with exceptionally high total cholesterol levels of at least 200 milligrammes per deciliter of blood, doctors may recommend one or more lipid-modifying drugs.
Statins are typically used to treat high cholesterol because they prevent the liver from producing cholesterol.
An additional medicine, such as: may be prescribed by a doctor if statins are unable to reduce LDL and triglyceride levels.
- Ezetimibe
- Niacin
- Fibrates
- Bile Acid Sequestrants
- Evolocumab And Alirocumab
- Lomitapide And Mipomersen
Prescription for Prevention
- Choose a plant-based, whole-foods diet that is high in fruits, vegetables, whole grains, legumes, fatty fish, nuts, and seeds, vegetable oils, and perhaps poultry or lean meat.
- Reduce amounts of higher-calorie foods and increase physical activity to maintain a healthy weight.
- Limit foods such fatty meats, butter, cheese, ice cream, other whole milk dairy products, egg yolks, solidified vegetable shortening, commercially fried foods, snack foods, and bakery goods that are high in saturated fats, trans fats, and cholesterol.
- Include modest amounts of foods such fatty fish, flaxseed, nuts, seeds, and liquid vegetable oils that are sources of unsaturated fats.
- Increase consumption of fruits, vegetables, whole grains, and high-fiber foods, especially oats, barley, and legumes.
- Limit consumption of high-sugar foods, such as fruit juices and sweetened beverages.
- To reduce blood sugar swings and regulate hunger, emphasise plant-based proteins (such as soy and legumes) and combine protein with carbohydrates during meals and snacks.
- If you do consume alcohol, do it in moderation.
- To further reduce cholesterol or TG, add plant sterols, viscous (soluble) fibre, and fish oil supplements as necessary.
- If the aforementioned actions do not provide sufficient control, add pharmacological medications.
Summary
The majority of individuals with hypertension also have concomitant dyslipidemia, and CVD risk factors are more frequently present in combination than alone. There is proof that dyslipidemia and hypertension together raise the risk of CVD. Clinicians should examine a patient’s overall ASCVD risk when contemplating cholesterol-lowering medication based on the ACC/AHA cholesterol treatment guidelines because many patients with hypertension who do not have increased LDL-C may benefit from statin therapy. Therefore, to maximise the reduction in CVD, a comprehensive strategy to CVD risk factor management is necessary, notably for hypertension and dyslipidemia. Even though certain anti-CVD drugs affect blood pressure and cholesterol, these effects are typically minor and outweighed by the decreases in CVD events.
Additionally, newer lipid-lowering treatments such PCSK-9 inhibitors demonstrate even higher lipid reductions without adverse blood pressure changes, effects that could lead to further decreases in ASCVD in a subset of hypertensive individuals with suboptimal lipid levels.
Get yourself check with INIGIMA online diagnosis a healthy step for longer life always connected with medical experts and doctors BOOK NOW
A review article by
Dr Bhavna Kalvala (Clinical Research Director @ IEEARC Tech)
Comments are closed